Interview
‘We can only solve this as a global community’
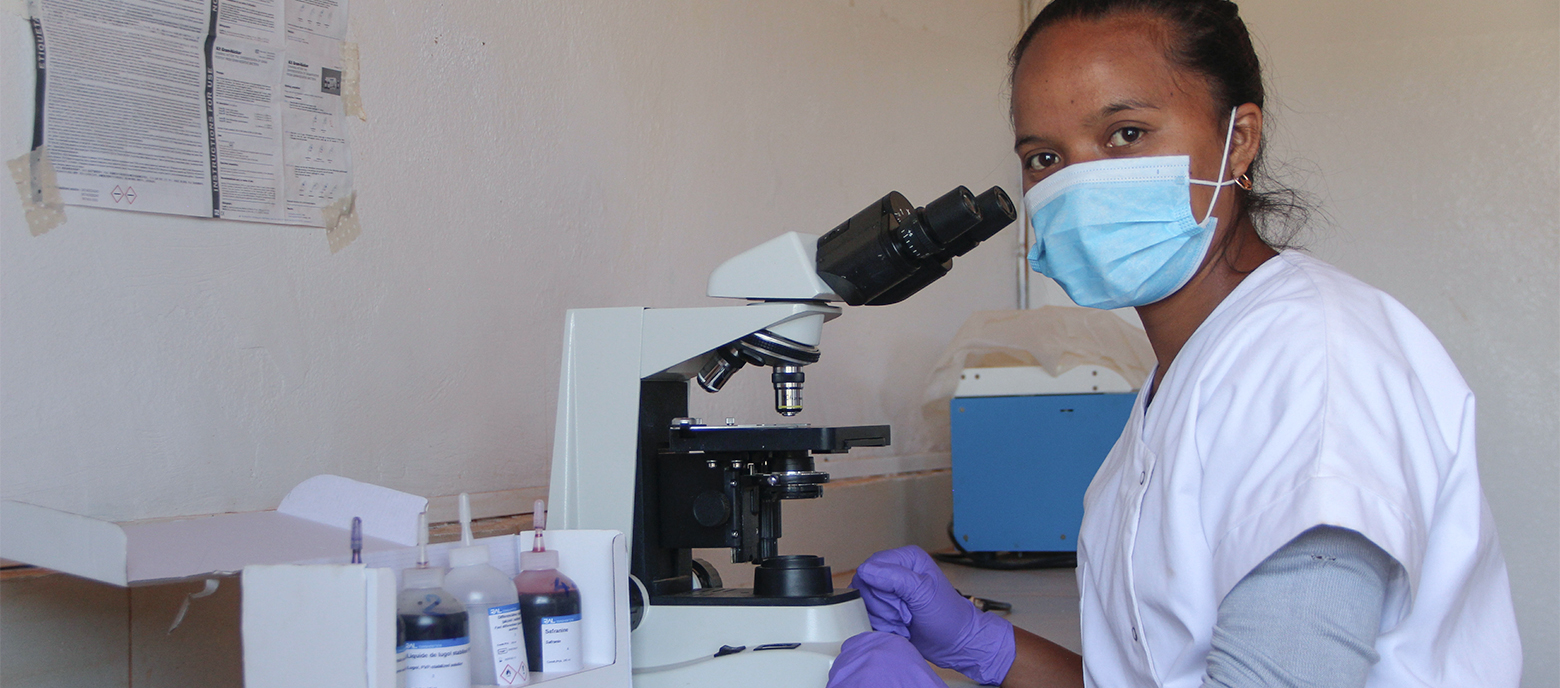
Microbiologist Michael Nagel has just returned from a challenging assignment in Benin. He is part of the German Epidemic Preparedness Team (SEEG), which was initiated by BMZ in cooperation with the Federal Ministry of Health in response to the Ebola crisis in West Africa. For the last five years, a core team based at GIZ has been monitoring reports of disease outbreaks worldwide and organising assignments at the request of partner countries. We interviewed Michael Nagel on SEEG’s current work:

Mr Nagel, how has SEEG’s work changed amid the Covid-19 pandemic?
We are receiving more enquiries than ever before. At the moment. These are primarily from Africa and Latin America – Guatemala, Peru, Bolivia, Colombia and Ecuador. However, the essence of our work has not changed. We are consulting with BMZ, and planning and implementing assignments worldwide.
How are you able to respond to this heavy demand?
We’re working under intense pressure. Our seven-member core team in Bonn comprises GIZ staff from various areas, including microbiology, medicine and global health. We are processing scores of enquiries, and organising and managing assignments. We usually receive support with this from experts from the Robert Koch Institute (RKI) and the Bernhard Nocht Institute for Tropical Medicine (BNITM). We have a formal cooperation arrangement with both institutes. Charité’s Institute of Virology in Berlin supported us with our work in Benin, West Africa, where we set up laboratory diagnostics to detect the Covid-19 pathogen. This was similar to the work we carried out prior to that in Namibia.
What were your assignments like?
In early March, it was not yet possible to test for the Covid-19 pathogen in Namibia’s national reference laboratory in Windhoek. The Namibian government responded at an early stage and asked us for assistance with capacity building. Shortly afterwards, I was able to travel to Namibia with a GIZ colleague, a colleague from RKI and a colleague from BNITM. Not only did we take testing kits with us, we also trained the laboratory personnel. This is a very important aspect, because everything needs to be set up correctly. Infection rates are determined in a country’s reference laboratory, and these figures are then reported to WHO. They are the basis for epidemiology and for decisions that governments take on mitigation measures.
You have just returned from Benin. What was needed there?
The assignment in Benin was very challenging. Although we knew the laboratory from previous assignments, this time we had to build up greater laboratory capacity there very quickly in order to make reliable diagnostics for the new coronavirus possible. The laboratory is actually designed for the detection of haemorrhagic fevers, such as Ebola or Lassa fever. Due to flight restrictions, we were only able to take a small team with us, meaning that the assignment had to be carried out with very limited resources. The GIZ country office gave us enormous support in this difficult situation.
Testing kits for the Covid-19 pathogen and protective equipment are in short supply. How are you dealing with this?
We only take protective equipment with us for personal use. When working in the tropics, masks need to be changed every two hours. We work in the laboratory for ten hours a day for around ten days. We also have testing kits with us for training and for the first few weeks. We then build contacts so that the laboratories can continue to be supplied with materials.
What has your work been like in the current pandemic. Has anything changed?
I have two small children and, in the current situation, my wife has to deal with everything when I am away. Just knowing that is a mental burden in itself. But the assignments are part of SEEG's work, it’s what we do. Of course, travelling is now much more difficult than it was at the end of last year when we went to Madagascar. We were only allowed to enter Benin at the personal invitation of the Minister of Health. We had to comply with strict regulations and could only board the plane if we had tested negative. We then had to provide evidence of three negative Covid-19 tests on site before we could start our work. And we only got seats on what is currently the last Air France flight to Benin through the German and French embassies.
What role do digital tools play given the travel restrictions?
We are currently developing webinars and are drawing on existing material. These online training sessions can provide a time buffer of weeks or months. If laboratory partners tell us that they can provide solid diagnostics, then this is an option. This allows us to respond to demand despite logistical difficulties. However, as soon as the travel restrictions are relaxed, we want to provide further training in person. That remains the gold standard.
When we look back on the current pandemic, what insights will have been gleaned?
I hope that governments and populations worldwide will recognise the importance of early warning systems and that the commitment to epidemic and pandemic preparedness need to be long-term. Prevention and, above all, health systems need to be strengthened so that they can respond appropriately to disease outbreaks. We can only mitigate the threat of pandemics in the long term as a global community.
April 2020